"My Story" by Tegan Cooke, Fashion Design Student Living With Fibromyalgia
Tegan is passionate about accessibility, sustainability, and hand-making production techniques as alternatives to fast fashion and as a fun way to prevent hand stiffness and discomfort. After hearing Tegan's inspiring interview with Mark Dennison on Radio Nottingham, Mary Fickling invited Tegan to share her story with the readers of PhysioPod NewsMagazine. Tegan has Fibromyalgia and is eager to raise awareness about it and other invisible disabilities.
MY EXPERIENCE OF FIBROMYALGIA
 My Experience of Fibromyalgia Audio
My Experience of Fibromyalgia Audio
As a young person interested in fashion, it can be really difficult when your chronic illness interferes with your ability to access exciting new clothes. So in my final year of my fashion design degree, I wanted to use my personal experience of Fibromyalgia to create adaptive clothing that alleviates the symptoms of my condition, rather than exacerbating them, whilst also celebrating all that I love about fashion.

I started to notice that something wasn’t quite right when I was in sixth form, that the way I felt was different to my peers. My joints clicked like theirs did, as we were all still growing, but I felt sharp pain each time which radiated throughout the affected area as a dull ache for ages afterwards. I could only do three days in a row at my after-school job before becoming exhausted, but my friend could do four days and be fine. And I, a straight-A GCSE student, was starting to struggle to concentrate in class and remember what we had learnt that day. The little things started to add up, until I was noticeably fatigued and in pain more days than not.
I had numerous doctor’s appointments and tests through a period of about a year, to try and find out what was wrong. More than once it was heavily implied that I was just growing or needed to be less stressed about my A-Levels. My symptoms reached the point where I couldn’t write notes in my classes without wrist supports and my teachers were having to put a plan in place to help me get through my exams. Then the country was put into lockdown.
I thought that maybe now school was done, my symptoms would improve, but nothing seemed to get any better, despite the days just lounging in front of Netflix or sunbathing in the garden. Fortunately with my mum’s persistence and advocacy, I was able to see a rheumatologist when the country started opening up again, who diagnosed me with Fibromyalgia (Footnote 1). I hadn’t heard of Fibromyalgia before this appointment, and neither did anyone else I knew. I learnt that it is a chronic condition characterised by widespread joint pain with no obvious cause, like inflammation or a broken bone, and fatigue even after resting. It is thought to be a problem with the central nervous system, so the messages sent to my brain by the nerves around my body are overactive, communicating pain where there shouldn’t be any. Suddenly things made sense to me – there was a name for this experience I was having, it was legitimate and real, not just in my head or an expression of exam stress.

Nottingham School of Art & Design, Bonington Building, Nottingham Trent University
I started studying fashion design at Nottingham Trent University not long after this diagnosis, having had very little time to learn how to manage my condition. I was juggling the usual worries around living away from home for the first time with anxiety about the worsening pandemic and my health struggles. It took me a long time to ask for help from the university and doctors, because in all honesty it took me a long time to accept that I was really struggling with this condition, and to admit that I couldn’t get through university on my own. Things started to change once I stood up for myself and asked for the help I needed, and I saw an improvement in my symptoms and my ability to manage them.
INSPIRED BY MY DISABILITY
 Inspired By My Disability Audio
Inspired By My Disability Audio
In my second year, I worked on a group project in the second semester in collaboration with the online retailer Very, with a brief to design a collection for people with disabilities that would fit in with what Very already sell. Although as a group we decided on a different part of the disability community to focus our project on, it got me thinking – could I look at my own disability in my final year? We were strongly encouraged by tutors to pick a topic for our final projects that we cared deeply about, as we would have to be working on it for about nine months. I wasn’t sure initially if I should look at Fibromyalgia or not – I was still grappling with the idea that my condition was ‘enough’ of a problem to be considered a disability. I was still wary of using the word ‘disabled’ to describe myself, and worried I was being over dramatic by identifying as such. I also knew if I looked at Fibromyalgia in my project, I would have to talk about it and my experience of it in my tutorial groups, with tutors and peers I didn’t know well, and share it publicly on social media or in my portfolios that I would use for job interviews, so I wouldn’t be able to avoid people knowing about my condition. After careful consideration, I knew I had to give it a go. If I could be brave and talk about Fibromyalgia, I could potentially make something that made a real difference to myself, but also to others with the condition.

So for my final major project for my Fashion Design BA (Hons) degree, I focused my project on Fibromyalgia, aiming to create clothing that benefitted those that suffered from the condition. I used my own symptoms and experience as my starting point for my design decisions, then surveyed nearly 100 people from around the world via social media to help understand how other people with Fibromyalgia (and overlapping conditions like Arthritis (Footnote 2), Ehler’s Danlos Syndrome (Footnote 3), and chronic fatigue (Footnote 4), feel, and particularly how clothes play a part in how they experience their disability. Initially I looked at existing items that can help ease symptoms to see how I could incorporate them into clothing, such as pillow sprays that make falling asleep easier, weighted blankets that also aid reduce anxiety, and the supports currently on the market that help ease joint pain. I also looked at crystals as my visual inspirations, as I thought about how a diamond’s beauty is formed under pressure and thought that fit very well with people who live with invisible struggles with their health.
WHAT I MADE
I had the option on my course to make only a few garments so that I could spend time properly developing and marketing them. My main piece is the weighted wrap coat, which is full of hidden adaptations, designed to support someone with Fibromyalgia.
- The wrap style is flattering to all shapes, so it can be worn by many people and can still fit comfortably even if the wearer’s weight or shape changes.
- The ties for the wrap are wide so they are easy to grab even with limited dexterity, which I made sure to test by tying it on days my fingers were at their strongest and weakest.
- The quilted shapes are a combination of classic diamonds and tracings of different crystals. I stuffed these by hand with weighted blanket beads, creating just enough pressure to aid pain relief and reduce anxiety. There was a lot of trial and error with this technique, but I really wanted to spend the time perfecting it, to explore how clothing could play a role in pain relief.
- I emphasised these stuffed shapes with hand beading and embroidery – celebrating slow craftsmanship techniques like embroidery is a personal passion of mine, and the antithesis to fast fashion. By using these techniques, I also wanted to showcase embroidery as a way of keeping your hands and fingers moving in a more fun way than physio exercises, which can often be boring and therefore aren’t done for enough time so don’t end up having much of a positive effect – I know I’m guilty of this! The beads also create texture and something to fiddle with, to again reduce anxiety and create positive sensations over negative ones for the wearer.
- There are some more quietly adaptive features too, including a lowered neckline and armholes to reduce how much sweat is visible on the garment, as struggling to regulate your temperature is also a common symptom of Fibromyalgia, and one that can make finding clothes to wear tricky.
- The lowered edges combined with the oversized fit make layering underneath easy, so if you need lots of layers or only one, you have the space to choose what goes underneath the coat.
- The edges of the coat are neatly bound and there is a smooth cotton lining, which both make sure there are no irritating seams or raw edges that may brush against the skin and cause irritation.
- The coat’s main fabric is a black bamboo/polyester blend. Using a blend of different fabrics brings out the best qualities of each one, making this fabric more breathable, soft, and sustainable than polyester on its own, and less easy to crease, more affordable, and less moisture (sweat) absorbent than bamboo normally is.
- The gathered high waist flows comfortably over the lower abdomen, hiding any bloating and allowing for weight fluctuation.
- The vibrant colours of the embroidery stand out, meaning the wearer isn’t hidden in plain and boring colours but can be loud and proud.
WRIST SUPPORT

This is an updated version of a typical elastic bandage wrist support, which normally appear medical and plain, and are often itchy and uncomfortable to wear. I’ve updated these in a fun purple, with neatly finished edges and a thumb, rather than a hole that digs in.
FUTURE
The adaptive fashion market has grown considerably in the last few years – even in the year since I started this project, we’ve seen UnHidden appear at London Fashion Week, the cover of British Vogue feature adapted designer fashion from brands like Erdem, and Channel 4’s latest show ‘The Unique Boutique’. From the beginning, my aim for my project was never to set up my own brand but to prove that adaptive fashion can and should be done. I would love to see it become more mainstream and not a niche little corner of the industry. Subtle features, like wider bows for ties or replacing tiny buttons with poppers or magnets, are so easy to achieve by any brand, from the high street to luxury, yet disabled people are still left out of fashion. I want the whole industry to think more about their customers, because disabled people want to be a part of fashion and should not be ignored any longer.
Transforming my project into a brand that sold carefully crafted pieces that aimed to alleviate symptoms of invisible disabilities would be incredible, but I think gaining some industry experience first is essential do doing this project, and my potential customer, justice. However, I’ve already gained so much from this project; my confidence in discussing disability as a whole and my personal experiences has grown so much, and I’m proud of how far I have come. I went from being worried about mentioning my disability, to talking about it live on local TV and radio. The most rewarding aspect of my project has to be these conversations. Getting more people to talk and to listen about this topic of invisible health conditions has been so informative, inspirational, and empowering – not just for me. I love that my designs have been a vehicle for these conversations, and I hope this is just the start for the visibility of invisible disabilities like mine.
To see more about my work or to chat to me about it, my website is www.tegancooke.weebly.com and my Instagram is @tegancookedesigns.
TEGAN COOKE
Website Instagram Email LinkedIn


1. What is Fibromyalgia?
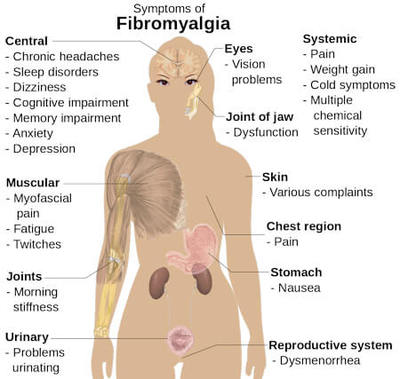
Fibromyalgia is a chronic disorder characterized by widespread musculoskeletal pain, fatigue, and tenderness in specific areas of the body. It is considered a central nervous system disorder, although the exact cause is still unknown. Common symptoms include excessive pain sensitivity, sleep disturbances, cognitive difficulties (often referred to as "fibro fog"), and heightened sensitivity to touch, light, and sound. Fibromyalgia can vary in severity and can be accompanied by other conditions like migraines, irritable bowel syndrome, and depression or anxiety. Treatment typically involves a combination of medication, therapy, lifestyle changes, and self-care strategies to manage symptoms and improve quality of life.
A pilot study carried out in 2013 (see references), concluded that "deep oscillation massage was shown to be safe and well tolerated in patients with moderate to severe grades of FMS of high chronicity and was highly accepted. The 3-month follow-up revealed sustained improvements in symptoms and quality of life, hence suggesting a benefit from treatment with deep oscillation massage, even though it was applied as a single-modality treatment. It also should be assessed whether vibration massage is a useful completion of aerobic exercise."
If you suspect you may have fibromyalgia, it is best to consult with a healthcare professional for an accurate diagnosis and appropriate management plan.
2. What is Arthritis?
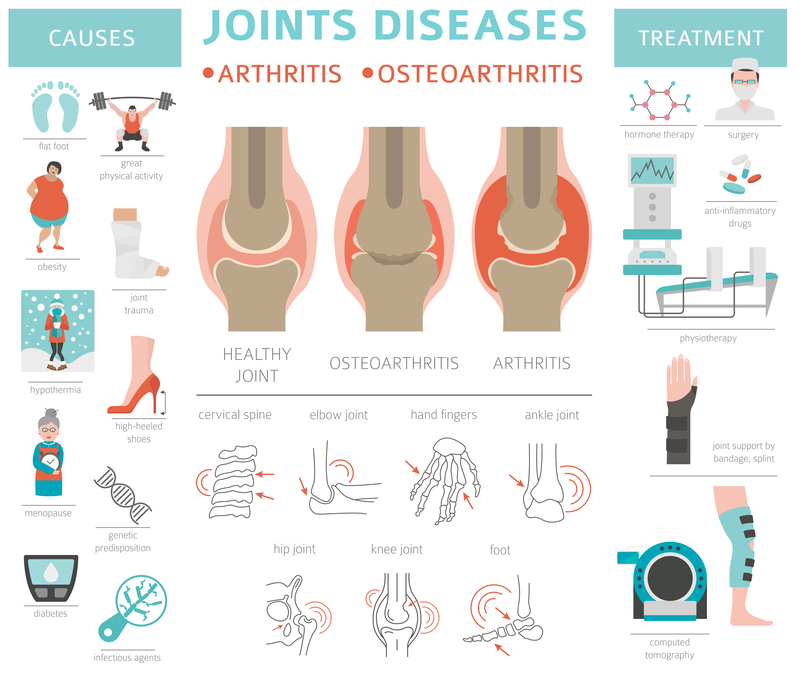
Arthritis is a term used to describe inflammation of one or more joints in the body. It is a common condition that affects millions of people worldwide. There are different types of arthritis, but the two most common forms are osteoarthritis and rheumatoid arthritis.
Osteoarthritis is a degenerative joint disease that occurs when the protective cartilage, which cushions the ends of bones, starts to wear down over time. This can lead to pain, stiffness, and reduced joint mobility, especially in weight-bearing joints such as the knees, hips, and spine.
Rheumatoid arthritis, on the other hand, is an autoimmune disease where the body's immune system mistakenly attacks the lining of the joints, causing inflammation, swelling, pain, and eventually joint deformity. It commonly affects the hands, wrists, and feet, but can also impact other joints in the body.
Arthritis can cause varying degrees of pain and discomfort, stiffness, and reduced range of motion in the affected joints. Treatment options depend on the specific type of arthritis and may include pain medications, anti-inflammatory drugs, physical therapy, lifestyle modifications, and, in more severe cases, surgical interventions.
In a study carried out in 2013 (see references) on the use of Deep Oscillation as an adjunct to kinesiotherapy in the treatment of Osteoarthrtisi results concluded "Before starting the treatment both groups behaved similarly, with moderate pain intensity, joint limitation and regular functional status, at the end of the treatment both groups evolved positively, with high percentages of satisfactory results (88 %) for those who received deep oscillation therapy."
If you're experiencing joint pain or suspect that you may have arthritis, it is important to consult with a healthcare professional for an accurate diagnosis and appropriate management. They can provide guidance and personalized treatment options to help alleviate your symptoms and improve your quality of life.
3. What is Ehlers-Danlos Syndrome (EDS)?
 What is Ehlers-Danlos Syndrome (EDS) Audio
What is Ehlers-Danlos Syndrome (EDS) Audio

Ehlers-Danlos Syndrome (EDS) is a group of genetic connective tissue disorders that affect the structure and function of collagen in the body. Collagen is a protein that provides strength and elasticity to various tissues, including the skin, joints, blood vessels, and organs.
There are several types of EDS, with different features and inheritance patterns. The most common type is called hypermobile EDS (hEDS), marked by joint hypermobility, joint pain, skin that is stretchy and fragile, and easy bruising. Other types of EDS may involve more severe symptoms, such as joint dislocations, skin abnormalities, vascular fragility, and internal organ complications.
EDS can manifest differently in each individual, even within the same family. Symptoms may vary in severity ranging from mild to potentially life-threatening. Some individuals with EDS may experience chronic pain, fatigue, musculoskeletal issues, gastrointestinal problems, and cardiovascular abnormalities.
Diagnosis of EDS often involves a detailed medical history, clinical examination, and genetic testing. Management of EDS typically focuses on symptom relief and preventing complications. Treatment may involve physical therapy, pain management strategies, assistive devices, and measures to protect vulnerable tissues.
It is important to consult with a healthcare professional specializing in genetic disorders or connective tissue disorders if you suspect you or someone you know may have EDS. They can provide a proper diagnosis and develop a tailored treatment plan to address specific symptoms and improve quality of life.
4. What is Chronic Fatigue?

Chronic fatigue, or chronic fatigue syndrome (CFS), is a complex and debilitating condition characterized by persistent fatigue or extreme tiredness that lasts for at least six months and is not relieved by rest. It is often accompanied by a range of other symptoms, such as cognitive difficulties (brain fog), unrefreshing sleep, muscle pain, joint pain, headaches, and flu-like symptoms.
The exact cause of chronic fatigue syndrome is unknown. It is believed to involve a combination of factors, including immune system dysfunction, hormonal imbalances, viral infections, and psychological stressors. Diagnosing CFS can be challenging, as there are no specific laboratory tests or biomarkers for the condition, and symptoms can vary from person to person.
Treatment for chronic fatigue syndrome is primarily focused on managing symptoms and improving quality of life. This may involve a combination of strategies, including pacing and conserving energy, cognitive-behavioral therapy (CBT), graded exercise therapy (GET), medications to address specific symptoms, sleep management techniques, and stress reduction techniques. It is important for individuals with chronic fatigue syndrome to work closely with healthcare professionals to develop an individualized treatment plan.
If you suspect that you are experiencing chronic fatigue or think that you may have chronic fatigue syndrome, it is recommended to consult with a healthcare professional who specializes in this condition. They can help evaluate your symptoms, provide an accurate diagnosis, and guide you in managing and coping with your fatigue.
REFERENCES

