Hands-On-Treatments and COVID19: Making It Work For The Client and Me
When lockdown happened back in March, I was just one week away from retiring from the best job I have ever had. I had only been with Mary Ann Evans Hospice for four years, but after twenty two years in Lymphoedema management, I now felt confident in my knowledge-base and skills. Finally, I believed in myself. That said, I have always believed in life-long learning and the specialism of Lymphoedema still excites me with research findings, new research projects and innovative approaches to help people living with lymphatic conditions.

Reaching 60 years of age marked a milestone for me. I loved the job, its challenges, the way innovation was embraced and encouraged. So different from the later years of my former clinical experience.
I knew I would miss the close-knit Lymphoedema team and the Hospice team as a whole. And of course, I would miss those patients who had allowed me to advise and treat them. I always feel it is such a privilege to be trusted to accompany someone on their journey through illness, recovery and sadly, sometimes through palliative stages and death.
But, my husband and I now had two young grandsons who lived some distance away and I really wanted us to be an active (and hopefully helpful) presence in their early years. I could easily carry on with First LymphCare, which I had established in 2003, seeing clients perhaps three days a week and spending a day each with my grandchildren.
In addition, I was negotiating some training for community home-care workers aswell as planning on-going mentorship and support for the Lymphoedema Team. And I was hoping to find time to return to poetry writing, sewing and wild swimming. The future was full of hope and excitement.
THEN... COVID-19 LOCKDOWN
.jpg)
COVID-19 infection rates spiralled world-wide and UK hospitals ramped up their response, all healthcare providers had to swiftly evaluate their own response. Like many others, Mary Ann Evans Hospice had to decide (if and) how they could continue to deliver care for those in need of end-of-life care, locally, while at the same time protecting staff, volunteers and the organisation. All a time of immediate loss of charitable income and a chaotic situation where PPE was in short supply for our staff. Nationally, outpatient non-essential services were stopped and this included Lymphoedema Services .
But it also meant that Independent therapists had to suspend work also. This was a legal mandate, but I had come to the same conclusion already as I listened to the daily Covid reports.
Suddenly, I was catapulted into a no-work situation. Not even private work. My Retirement day at home in isolation was distinctly odd and sadder than I had anticipated. And so empty.
The first thing I did was contact all of my regular clients to check how they were and if they needed anything. I reassured them that they could contact me any time if they had any issues regarding their Lymphoedema. For some that contact was enough, for others I made video calls, so that I could visually assess specific problems they were having, and then advise appropriately.
I started to write advice on my Facebook First LymphCare page and Website. And I resolved to use the time to continue learning . Many of the medical companies put on high quality online discussions and learning. I attended training online thanks to: Thuasne, Juzo, Physiquippe, Jobst and Haddenham Healthcare, Lymphoedema Training Academy and I greatly appreciated having the time and energy to participate and broaden my knowledge. I did online courses with the BMJ, LinkedIn and I took part in interactive discussions for Alzheimer’s Society.
Gradually, I started to plan for the moment when the government would ease working restrictions and permit hands-on therapies once more. It would be vital that I had robust policy and procedures in place. It is a huge responsibility as an Independent Nurse and Therapist, to ensure that EVERYTHING relating to a client attending for and having a treatment, is as covid-safe as possible. The buck stops with me!
So, it was important that I equipped myself with the right knowledge, the best advice and that I would fulfil the requirements of: the NMC, RCN, FHT, my insurers and of course legislation.
I found an excellent, detailed and thorough course specifically for therapists. And was pleased to gain Certification in Preventing Cross Infection in a post-covid world from the Jennifer Young Training school.
RETURNING TO FACE-TO-FACE TREATMENTS
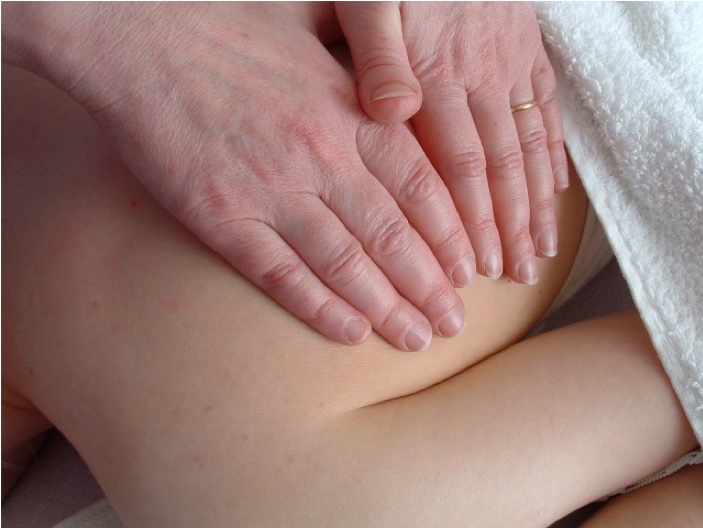
For me, that long period of non-contact, came at the end of July when our government finally gave the go-ahead for face-to-face manual therapies to resume. Before this date, therapists who continued to work may well have not been covered by their governing bodies or their insurance. I was not prepared to compromise my patients’ safety, or my standards, so used the time to study all aspects of safe covid-19 working and to formulate my own protocols and procedures.
I wanted to be confident that when clients attended for appointments, they would feel as safe as possible at First LymphCare. But also, that I personally, and my household were also safe, since my clinic room is attached to my home.
I scrutinised every aspect of an appointment, from first contact (virtual), through arrival, assessment, treatment, payment and departure. I would advise every therapist to do this: it gives a new insight into what we, as face-to-face practitioners do and is a good way to evaluate effectiveness and practice. From this analysis I was able to create a formal policy and set out new procedures and ways of working.
Policy and procedures ready, I enlisted my regular clients to read and evaluate my plans and to add their own thoughts or suggestions. There was a unanimous 'thumbs up'!
Next step was to make a public statement on my website and FB page that I was taking appropriate steps to keep my practice safe.
SO, WHAT DID I CHANGE?
I sewed pretty three ply face coverings and sent one to every client on my books. This reassured them that I was still there for them and also underscored that they would be expected to wear a covering at future appointments. The response was 100% positive.
- Pre-appointment checks: Day before or morning of appointment client receives text from me confirming my covid-free status/ no contacts etc and they reply confirming theirs. Any possible symptoms in either party means appointment will be deferred.
- Arrival. I (in mask) meet client( in mask) at side access*, and lead directly into treatment room, where they hand sanitise.
- *Access. We had to make the footpath safe, add outdoor lighting, and safety markers for steps. In winter I will need to ensure it is de-iced and gritted.
- Ventilation: Window is always slightly open to allow airflow.
- Infection Control: Wipe clean chair for client and wipe clean box in which they can place handbags, coat, clothes.
- Preserving Dignity: No soft coverings on couch now I made thin cotton 'dignity' coverings for during treatments which can be washed at high temperatures. (No cosy blankets now)
- Step, scales and all equipment are easy to clean and sanitize after each client.
- Hydration: Paper cups for water/client brings own drink.
- Payment: Clear plastic wallet for cash payments or prepaid via bank transfer.
- Toilet facilities:Separate toilet used only by clients. Paper towels only.
- Personal Protective Measures: Clinician wears gloves, mask and visor for facial and upper body treatments, and gloves and mask for lower body treatments. Clean scrubs set for every patient.
- Personal Protective Measures: Patient wears mask throughout treatment, (unless facial oedema).
- No co- attendees.
- Case load: one client a.m., one client p.m. and one evening client. This allows me time to decontaminate the room, the equipment, and air the room between clients.
HOW HAS IT GONE?
Very well actually. I'm pleased to say that clients have all said how comprehensive my procedures are and this makes them feel safe. They really appreciate the pre-appointment contact and accept that appointments may need to be deferred at short notice.
Mrs A wrote: ‘An added measure is the pre-appointment protocol of texting to advise that she is well and covid free and enquire if I am also well. This further reassures me that she’s doing all that is necessary to keep both clients and herself safe.’
The checklist I have developed for decontamination and cleaning of equipment and the room itself ensures that all areas are cleansed. And I now have my deep clean routine finely tuned.
Everyone wears a mask without complaint and although history taking is a little more difficult and takes a little longer, it is not a problem.
NEGATIVES? Surprisingly Very Few...
Wearing glasses, a visor and a mask can make it very hot when treating patients and at times my glasses or visor steam up.... but it's manageable.
Green planet considerations
I decided against constantly using plastic aprons. Early on, I struggled to buy them. Then I decided that I didn't really want to add to plastic waste unnecessarily. So, I made three ply re-usable cotton masks and use lightweight cotton scrubs, changing for each patient. It works surprisingly well.
How has COVID 19 impacted on clients?
Initially, patients already diagnosed with Lymphoedema, who had been seen by a clinic, were confident in self-management. However, as time goes on with many services re-starting, patients are becoming anxious and searching for advice and reassurance via social media.
More people with Lymphoedema, or suspected Lymphoedema and Lipoedema are self-referring and clients travel significant distances for me to treat them. This is a worry, as clearly the more local your treatment the better.
I have always taught people living with Lymphoedema how to self-manage their condition, but the need for this is even more apparent. I am dumb-founded at times that people have not been taught SLD, or shown how to apply garments correctly.
Sometimes when patients have always had garments supplied by a clinic, they are now realising that they have no idea how to access replacements, (even when these are
prescribable off the shelf items). Why is this?
It's great that services can give hosiery to patients, but if the clinic has created a dependency for garment replacement, then the patient is not being empowered to self-manage. This is a dis-service to the patient and not best practice. I am finding that Covid 19 has exposed the disparity in service provision, and also in the quality of the actual interventions provided pre-covid.
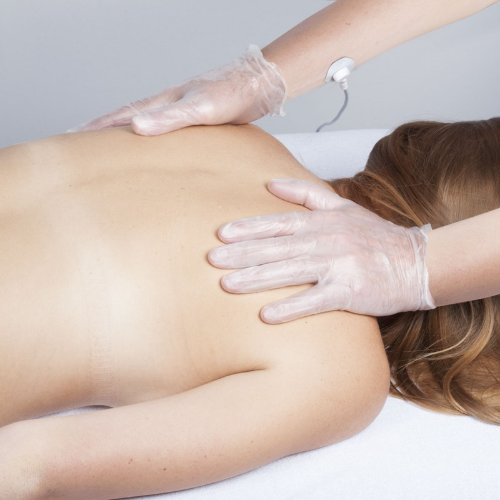
DEEP OSCILLATION (ALREADY HYGIENICALLY APPLIED) THROUGH VINYL GLOVED HANDS
Aesthetic surgeons have now resumed their work, and First LymphCare receives increasing enquiries for post-surgery MLD and Deep Oscillation therapy. And I have also had a number of new referrals of people who have surgery planned for treating Lipoedema or joint replacement surgery. Again, Deep Oscillation comes into its own for post-operative recovery and pain relief.
Retirement going to plan now?
We’ve been to our beloved Lake District, gone fell walking and wild swimming, grown vegetables, penned a couple of poems and have enjoyed zoom tea times and play times. Our extended family have been very stringent in our social distancing. Our first socially distanced days with each family was in July and two weeks ago we had our first contact with our youngest, picking him up from a stumble making sure he faces away from us. We don’t kiss or cuddle and keep fully distanced from their parents at all times. But….. it is so special that we can actually see them, interact with them.
So, all in all, after six months without work, doing hands-on therapies in a world still under the spectre of COVID 19, is a challenge, but is do-able and is as enjoyable and rewarding as it ever was. Retirement is going well!

Sue Hansard
Lymphoedema Nurse Specialist.
First LymphCare

