Finding Balance: A Compassionate and Clinical Guide to Alcohol and Lymphatic Health by M Fickling
Discover the latest clinical insights on how alcohol truly affects the lymphatic system, exploring everything from the "dehydration-retention paradox" to the hidden impact of liquid calories. This compassionate, evidence-based guide empowers those living with lymphoedema to understand their bodies and make informed lifestyle choices without guilt.
Living with a chronic condition like lymphoedema requires a relentless, exhausting daily commitment to your body. Between meticulously applying compression garments, performing lymphatic drainage, and constantly monitoring your skin, it is entirely understandable that many people turn to a glass of wine or a beer simply to relax, unwind, and recapture a sense of normalcy at the end of a long day (Ercolano, 2017; Macmillan Cancer Support, 2023).
However, many patients notice that their compromised lymphatic systems struggle to process these beverages, leading to mysterious "lymphie hangovers" characterised by profound heaviness, nausea, and throbbing headaches after just one or two drinks (UmLydia, 2024). If you have experienced this, it is not your fault. Looking at the latest clinical science allows us to understand exactly how alcohol interacts with your lymphatic system—not to induce guilt, but to empower you with the knowledge to make compassionate, informed choices for your body (Academy of Lymphatic Studies, n.d.).
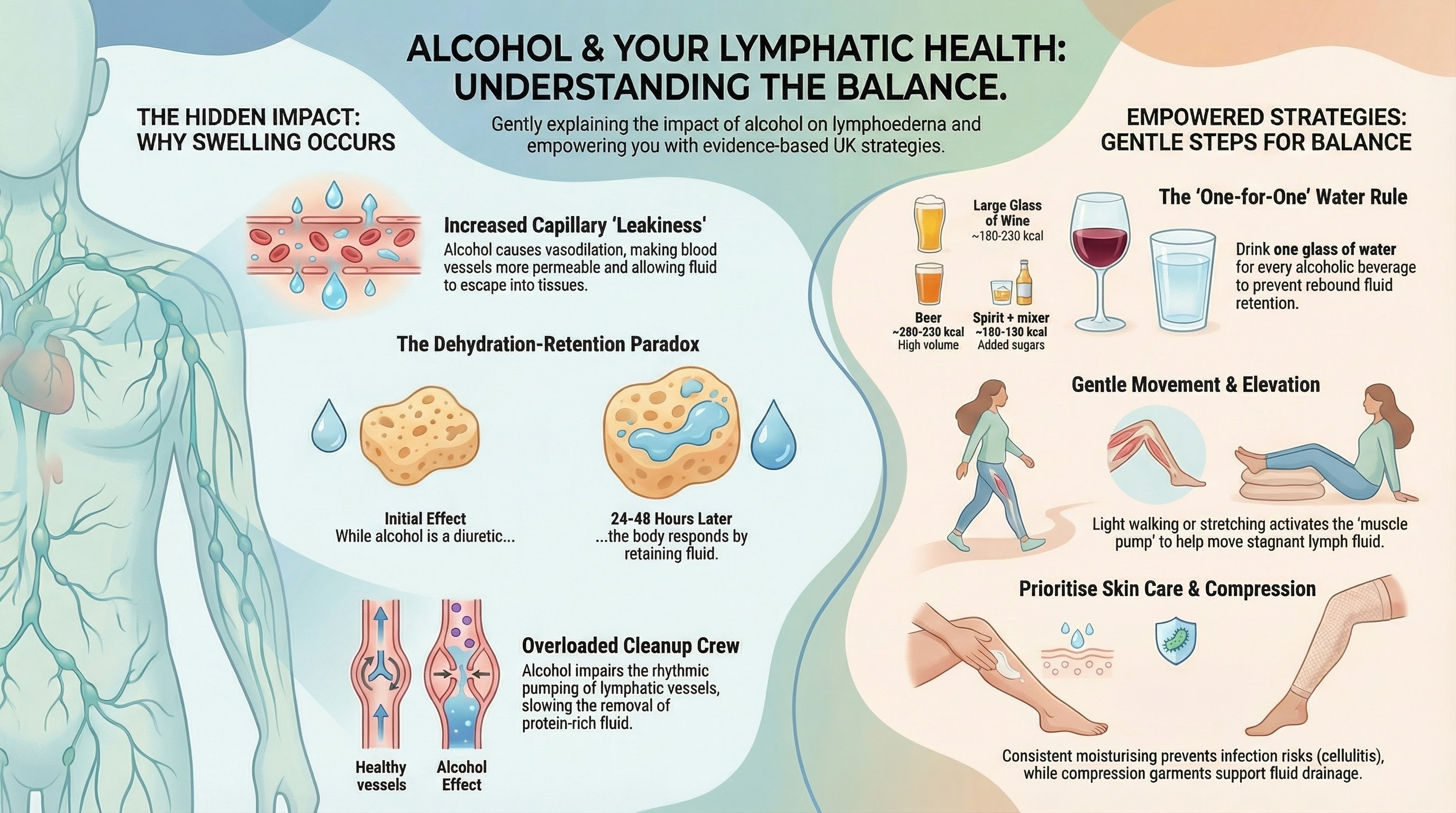
Hemodynamic Shifts and the "Leaky Vessel" Effect. From the very first sip, alcohol acts as a systemic vasodilator, causing the smooth muscles of your blood vessels to relax and expand (Ercolano, 2017; Drisdelle, 2021). While this creates a warm, relaxing sensation, it significantly increases blood flow to the skin and peripheral tissues, forcing more fluid to filter out of the capillaries and into your tissue spaces.
Clinically, a single dose of alcohol has been shown to increase thoracic duct flow by 22%, which can rapidly raise the volume of an affected limb by 8% to 12% (Acibadem Health Point, n.d.). At the molecular level, alcohol disrupts VE-cadherin, a vital tight junction protein that maintains endothelial cell integrity. This disruption severely weakens the vascular barrier, leading to a 300% increase in fluid and protein leakage (extravasation) into the surrounding tissues (Acibadem Health Point, n.d.). Furthermore, chronic alcohol use reduces hepatic lymph protein levels by 27%, creating a severe osmotic imbalance that overwhelms an already struggling lymphatic system (Acibadem Health Point, n.d.; Kondo & Iwakiri, 2020).
The Dehydration-Retention Paradox One of the most frustrating mechanisms of alcohol is the "dehydration-retention paradox" (Academy of Lymphatic Studies, n.d.). Because alcohol is a diuretic, it forces your kidneys to excrete more water (Drisdelle, 2021). While you may initially feel like the alcohol is "drying out" your swelling, the fluid lost is primarily water, leaving behind a highly concentrated pool of proteins trapped in your delicate tissue spaces.
Because these proteins act like sponges, your body senses the dehydration and triggers a potent hormonal response to retain water intensely over the next 24 to 48 hours. This draws even more fluid back into the affected limb, which scientifically explains the delayed, painful swelling flare that often occurs the day after drinking.
Immunological Sabotage and the Threat of Cellulitis. Lymphoedema already places you at a higher risk for cellulitis, an acute bacterial skin infection that can cause irreversible scarring to your lymphatic architecture (BLS & LSN, 2025). Unfortunately, alcohol critically sabotages the immune system’s ability to fight these infections (Banyan Treatment Center, n.d.).
Binge drinking directly elevates pro-inflammatory cytokines, and chronic consumption dangerously impairs leukocyte (immune cell) recruitment to the tissues (Pascual et al., 2017; Mathis et al., 2007). Furthermore, alcohol compromises the formation of neutrophil extracellular traps (NETs), which are essential for trapping and killing bacterial invaders (Wang & Tian, 2018).
The clinical impact of this immune suppression is severe: alcohol elevates perilymphatic TNF-α (a major inflammatory marker) by 45% and causes D6 receptor dysfunction, which prevents your body from clearing out inflammatory molecules (Acibadem Health Point, n.d.). This systemic vulnerability explains why the annual risk of cellulitis doubles for those having more than three drinks a week, and why long-term use suppresses VEGF-C (a protein vital for lymph vessel function) by 38% (Acibadem Health Point, n.d.).
Metabolic Impacts: Being Gentle With Your Weight. Maintaining a healthy weight is incredibly difficult with lymphoedema, and it is vital to be gentle and patient with yourself on this journey (L-W-O Community, 2026). Scientifically, however, obesity and adipose tissue deposition (ATD) mechanically impede lymphatic drainage and produce inflammatory cytokines that worsen swelling (Fletcher et al., 2025).
Because alcohol is calorically dense, it provides "empty calories" that can quietly contribute to weight gain and place a heavier mechanical burden on your lymphatic system (L-W-O Community, 2026). To protect your overall health, the American Cancer Society and American Institute for Cancer Research recommend avoiding alcohol or limiting it to one drink per day for women and two for men (University of Miami Health System, n.d.), while UK Chief Medical Officers strongly advise keeping intake below 14 units per week (GOV.UK, 2025).
Empowerment Over Guilt. If you choose to enjoy a drink, there is absolutely no need for guilt. The goal is to use this clinical knowledge to practice proactive self-care. You can mitigate these physiological responses by pacing your drinks with plenty of water to prevent the dehydration-retention rebound, engaging in gentle movement the next day to activate your muscle pump, and wearing your prescribed compression garments to support your vessels against fluid leakage (Ercolano, 2017; Academy of Lymphatic Studies, n.d.). Ultimately, true control over lymphoedema begins with self-compassion and understanding exactly what your body needs to thrive.
Glossary of Clinical Terms
- Adipose Tissue Deposition (ATD): The accumulation of fat cells in the body, which can physically compress lymphatic vessels and produce inflammatory signals that worsen lymphoedema.
- Cellulitis: An acute, spreading bacterial infection of the deep skin tissues characterised by pain, warmth, swelling, and redness, which can cause permanent damage to lymphatic vessels.
- Dehydration-Retention Paradox: A physiological response where diuretic fluid loss (such as from alcohol) leaves behind high protein concentrations in tissues, causing a delayed hormonal rebound that attracts more water and worsens swelling.
- TNF-α (Tumour Necrosis Factor-alpha): A pro-inflammatory protein in the body. Alcohol significantly elevates perilymphatic TNF-α levels, thereby worsening tissue inflammation.
- Vasodilation: The widening and relaxing of blood vessels, which increases blood flow but allows more fluid to leak into the surrounding tissues.
- VE-cadherin: A vital tight junction protein that maintains the structural wall of the lymphatic and vascular endothelium. Alcohol disrupts this protein, causing the vessels to become "leaky."
- VEGF-C (Vascular Endothelial Growth Factor C): A protein essential for the growth, function, and survival of lymphatic vessels. Chronic alcohol use suppresses its production.
Scientific References
- Acibadem Health Point. (n.d.). Can You Drink Alcohol with Lymphedema? Expert Advice.
- Academy of Lymphatic Studies. (n.d.). Alcohol, Inflammation & Lymphatic Drainage: What Actually Happens.
- Banyan Treatment Center. (n.d.). Cellulitis and Alcohol Risks.
- British Lymphology Society (BLS) & Lymphoedema Support Network (LSN). (2025). Guidelines on the Management of Cellulitis in Lymphoedema.
- Department of Health and Social Care. (2025). Delivering better oral health: an evidence-based toolkit for prevention (Chapter 12: alcohol). GOV.UK.
- Drisdelle, D. (2021). How Alcohol Affects Your Lymphedema. Flow Lymphatic Health Clinic.
- Ercolano, A. (2017). Bottoms Up! The Effects of Alcohol on Lymphedema. The Lymphie Life.
- Fletcher, J., Borthwick, Y., Brown, L., et al. (2025). The impact of obesity on lymphoedema. Wounds UK.
- Kondo, R., & Iwakiri, Y. (2020). The lymphatic system in alcohol-associated liver disease. Frontiers in Physiology, 11, 574607.
- L-W-O Community. (2026). Healthy Eating.
- Macmillan Cancer Support. (2023). Understanding lymphoedema.
- Mathis, K. L., Stokes, K. Y., & Granger, D. N. (2007). Chronic alcohol consumption impairs leukocyte recruitment and promotes endothelial cell apoptosis in the mesenteric microcirculation. American Journal of Physiology-Heart and Circulatory Physiology, 292(1), H587–H595.
- Pascual, M., Montesinos, J., Marcos, M., Torres, J. L., Costa-Alba, P., García-García, F., & Guerri, C. (2017). Gender differences in the inflammatory cytokine and chemokine profiles induced by binge ethanol drinking in adolescence. Addiction Biology, 22(6), 1829–1841.
- Szabo, G., & Saha, B. (2015). Alcohol's effect on host defense. Alcohol Research: Current Reviews, 37(2), 159–170.
- University of Miami Health System. (n.d.). Nutrition for Lymphedema. Sylvester Comprehensive Cancer Center.
- Wang, H., & Tian, Z. (2018). Alcohol compromises neutrophil extracellular traps through upregulating IL-33 expression to increase susceptibility to bacterial infection. Frontiers in Immunology, 9, 1322.
Author's Note: This article was written by M. Fickling with research, structuring, and drafting assistance provided by an artificial intelligence (AI) tool.
How to cite this article: Fickling, M. (2026). Finding Balance: A Compassionate and Clinical Guide to Alcohol and Lymphatic Health. PhysioPod® UK.

